
Last year, the number of GPs in England fell by more than 1,000 – and a record number of surgeries closed. Earlier this year, the largest annual survey of GPs found that unfilled vacancies were at their highest ever level. There is a national shortage of GPs, and the situation is getting worse. So what’s going on?
I recently spent three days at the Lambeth Walk Practice in Kennington talking to staff and patients and watching the team at work to try to understand some of the pressures general practice is facing after seven years of austerity. I wanted to see what effects the cuts have had on both the surgery – and the community it serves…
IT’S JUST getting light as I arrive at the surgery. It’s 7.03am on a chilly October Monday and I’m late for my first day at the Lambeth Walk Practice in Kennington. Dr Raj Mitra, who I’ll be spending the next 11 ½ hours with, is already seeing his first patient. Three more are sat in the waiting room and receptionist David Vizuete, who’s been here since 6.30am, is the lone presence the other side of the counter.
Raj and his practice have been installed in this handsome art deco building – a former wash house – since 1995. Lambeth Walk was once a popular shopping street with a famous market, but the area was devastated by bombing during the Second World War and never recovered. Many of the buildings that survived the Blitz were torn down in a wave of redevelopment and replaced with large housing estates.
Behind the surgery the skyline still bulges with one of the more successful examples of this: Lambeth Towers, the concrete embodiment of architect and social housing pioneer George Finch’s vision for a more egalitarian system of housing, completed in 1972. Behind that lies the Imperial War Museum, with St Thomas’ hospital, the Thames and Parliament just a few hundred metres to the north.

Despite its proximity to Westminster, and a few wealthier streets lined with large Georgian houses, this is still a very poor part of London. Remarkably, it has stubbornly resisted much of the aggressive redevelopment engulfing the surrounding areas.
In Elephant and Castle, just a ten-minute walk from here, generic glass and steel towers, packed with luxury apartments and little or no social housing, have swept away many of the 1960s estates. Their residents have been forcibly displaced in the process, whole communities violently uprooted and scattered to the fringes of London and beyond to make way for overseas property investors – perhaps most famously with the demolition of the Heygate Estate in 2014.
For now, the estates that surround Lambeth Walk have survived, an increasingly isolated enclave of the old London. Warning signs abound, however – two new upmarket hotels have sprung up just over the road and a 22-story block of eye-wateringly expensive flats looms imperiously over Lambeth North tube station. There can be no doubt that developers are waiting in the wings, itching to dismantle George Finch’s dream.
Residents of the two largest estates – China Walk and Ethelred – still make up the majority of Raj’s patients, although this is changing, he says. One of the locums who also works at a surgery just a couple of hundred metres closer to the river tells me that the patients she sees there are now primarily wealthy, middle class professionals. The original residents are disappearing.
I’ve come to Lambeth Walk to spend three days with the doctors, nurses, support staff and patients. I want a glimpse of life in a modern GP surgery, to understand the role it plays in this community and, crucially, to see what effect Government cuts are having on the practice, on the NHS more broadly – and on the patients themselves.
***
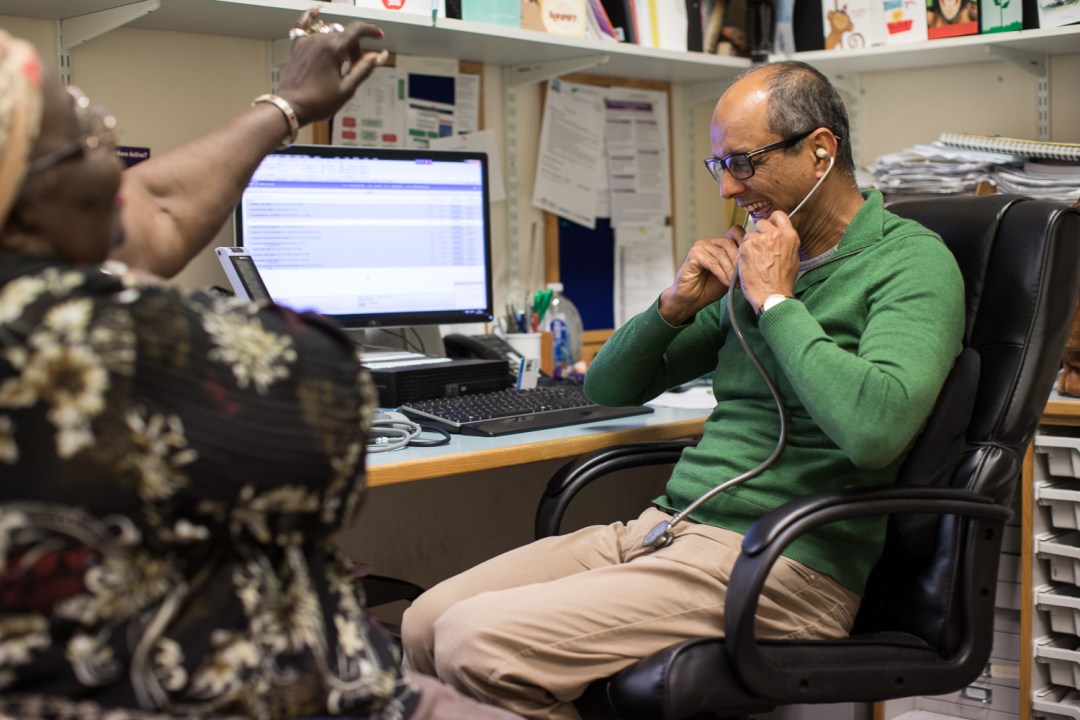
It’s going to be a busy morning, Raj warns me, when he emerges from his first appointment and invites me into the consulting room. One of the nurse practitioners is off sick and Mondays are usually the most hectic days, so the team will see more patients than usual.
Despite the age of the building, and the fact the surgery hasn’t been redecorated in a few years, his room feels spacious and light. At one end is the examination table and a sink. A blue privacy curtain cuts the space in half and at the other end are his desk and two chairs for patients. The shelves above his computer are stuffed with books, periodicals, folders and thank you cards – the latter from patients and some of the surgery’s regular student doctors. Photographs, flyers, certificates and children’s drawings adorn the walls. He has a cupboard full of gifts from patients. Raj has been treating people in this room for a long time.
“When I first came here, I was seeing the old Londoners,” he tells me. “I had one patient who was 108, born in 1892.” Originally from Essex, he bought a house in the area when he arrived and has lived here ever since – something he says is no longer an option for the younger doctors at the surgery. “These days you’re looking at £400,000 for a small ex-council flat around here. More.”
I ask why he chose Kennington. “I could have worked in the countryside and had an easy life,” he says. “But I became a doctor because I wanted to make a difference, and I thought I could do that here. I wanted to live and work in my community.”
They open the surgery early at least twice a week to cater for the large number of patients who work anti-social hours, often in low paid jobs. The person I just missed was an office cleaner, he says.

I spend most of the day with Raj in his consulting room – breaking briefly for coffee and a short lunch. By 4pm he’s seen 29 patients. Two others fail to turn up and he phones them, initially to check they’re ok and then to chastise them for wasting valuable slots. He explains that the rest of his day is spent writing up notes and reports, making calls, sending faxes and emails, writing letters on behalf of patients, writing referrals, checking in on the student doctors and working with Sarah, the practice manager, to make sure the surgery is generally running well. There’s a lot to keep on top of.
The reasons that bring people to his door today vary, but mental health and obesity-related issues are the most common. “Mental health is the number one thing we see now,” he says. “A lot of obesity as well – and they’re often linked to poverty. All our rich patients are thin. It used to be the other way around.”
One of the first patients in the morning session is a woman in her 50s who Raj has known for years. She tells us that she’s been feeling down recently. She has a history of depression, anxiety and panic attacks and struggles with her weight. She’s in the early stages of the menopause and is having problems sleeping as a result. She lives alone and rarely leaves her flat these days, she says.
She explains that she finds reading and writing difficult, and this contributes to her isolation.
Raj is clear – she has to get out more often. She needs to plan activities. He gives her flyers for gardening and weekly wellbeing groups that the surgery offers. There’s an exercise class nearby run by a charity that he points her to. He also suggests counselling – but explains that there’s currently a three-month wait.
She needs to build up her confidence, he says, and to be able to get back to work. She seems cautiously positive at the idea of the groups. “It’ll give me something to do,” she says. Raj asks her to come and see him again in a month to check how she’s getting on.

A little later we meet a woman in her late 60s with mobility issues. She has severe arthritis, particularly in her back. She’s retired but says she’s bored and lonely. Lots of the services that used to exist for elderly people in this area have been cut. This is something I hear again and again from the older patients I talk to – and they spend more time alone at home as a result. The surgery set up the gardening and wellbeing groups to try to fill this gap.
I ask Raj what he’s seen change in his 22 years here. Is it busier? “It’s always felt busy,” he says, “but 20 years ago I had longer lunches! I do a lot more phonecalls now, fewer home visits. Each person has more than one problem and often they’re quite complex. I see people more often. Back then the average consultation rate [per patient] was three over a year – now it’s six. The internet is part of that, but it’s also people living longer, cancer survival rates improving. We’re much better at keeping people alive now.”
And what about the cuts? What’s changed since austerity was announced in 2010? “Well, I’m giving out lots of foodbank vouchers,” he says, “often because of benefit cuts. I see lots of benefit reviews, with more and more people getting denied – often people with quite severe long-term illnesses and particularly people with mental health problems.”
“I’ve seen a significant reduction in social services provision,” he continues. “And the threshold [how severe your situation has to be before you can get help] is rising. Waiting times for A&E and outpatients have gone up.” He pauses to think. “That’s certainly some of it. There’s a lot.”

After lunch I’m introduced to a 46-year-old woman who suffers from chronic schizophrenia. She was working as a carer, but had to stop when her condition worsened. She tells us that she’s still hearing voices and isn’t sleeping. “When I watch TV they talk back to me,” she says.
She’s frightened of taking her medication because one side effect is that it contributes to her obesity. She explains that she’s signed on, but is currently getting no benefits and is surviving on her savings – which are fast running out. Raj refers her to the Community Mental Health Team and says he’ll write a letter to the Department for Work and Pensions (DWP) for her.
We meet one man in his late 30s who Raj has been treating since he was a teenager. He has diabetes and has suffered from obesity and depression in the past. He explains that he was very unhappy a few years back after the breakdown of a relationship. He eventually lost access to his children.
Today the news is good, however. He’s lost weight, he’s seeing his kids again and he’s found a new partner. He’s here because he suffers from sleep apnoea and needs Raj to write a report for him to the DVLA before he can start driving again. While he’s there, Raj gives him a flu jab. They talk as friends and Raj is clearly delighted to see him doing so well.

One of the last patients of the day is a softly spoken young man who has had problems with his mental health since he was a teenager. He tells us something of his very challenging upbringing and says that he’s been self-harming since he was 15. He’s begun again recently.
He speaks eloquently and frankly about going in and out of depression, how he struggles to control his anger – and the effect it has on those around him. He says he’s seen a few doctors over the years, but has mostly felt fobbed off. Raj talks to him for a long time – I lose track, but it’s a lot longer than the allotted 10 minutes. Eventually he refers him for therapy, prescribes anti-depressants, encourages him to exercise and offers some advice to help him sleep.
***
It’s striking how many of the people we see have been coming to Raj for years. Some bring presents and news of the grown-up children he’s known since birth. There’s a lot of warmth – hugs, hands on shoulders, handshakes. I spend much of my second day in reception, talking to patients in the waiting room, and many of them – most of the older patients, in fact – have come specifically to see him.

These are people who have a relationship with their GP – someone who doesn’t have to look at a computer to know their medical history. Convenience counts for so much in the modern world that I hadn’t realised how comparatively transactional my dealings with GPs have become.
At my surgery I have rarely seen the same doctor twice in the 11 years I’ve been registered. That’s partly because it’s a large practice with a high turnover of staff, but it’s also down to my impatience, my expectation – fostered in a culture of instant gratification – that I must see someone, anyone, immediately, however minor the ailment may be.
Raj explains there is a financial cost to this: less experienced doctors who don’t know their patients tend to over-refer – to err on the safe side, essentially. A GP who has known a patient for many years is in a better position to judge what is really needed, he says, and that can save the NHS a lot of money, especially in an era where people diagnose themselves online before an appointment, and it can be easier just to give them what they think they need.
***
In reception I chat to Dora, who registered the year Raj arrived. She’s come to see him again today. “He’s very good,” she says. “He’s been my doctor for a long time, so he really knows me. He’s known me from when I was well to now. He understands.” I ask if she’s noticed any changes since the cuts began. “There used to be lots of places where children could go out and play, but most of those have gone now, they’re flats. And everything takes longer – hospital appointments take months.”

Next I talk to Patsy – also here to see Raj – who moved to Kennington in 1978 and has been coming to this surgery ever since. Back then it was in a different building, she explains.
I ask what she’s seen change more recently. “A lot of places have been pulled down around here,” she says. “Denby Court [a sheltered housing block for elderly tenants] has gone. We used to have another place where we did tai chi, played bowls and had exercise classes, but Lambeth took the funding away a few years ago. It was a social place. If someone didn’t turn up, you’d find out what had happened to them. Now you just don’t know.”
She tells me that she worked in an NHS clinic around the corner for 26 years until she retired. It was sold off in 2014 and is now a privately owned medical centre where disability benefits claimants are assessed.
I meet three generations of one family – Hetty (grandma), Lynda (mum) and Dionne (Lynda’s grown up daughter). All are here for their flu jabs. They’ve lived in the area their whole lives and have been coming to this surgery long before it moved into the wash house.

I ask them the same question. “A lot of the libraries have closed down,” says Lynda. “There was a luncheon club for the elderly that’s gone. And at St Thomas’ the waiting times are much longer. You notice it in A&E. They’re under a lot of pressure. They kept Dionne in overnight just because no one could see her until the next day. She was taking up a bed unnecessarily.”
***
Kate Pattle is one of Lambeth Walk’s locum nurse practitioners, and has been working at surgeries in the area for many years. She cares for her elderly mother, which is why she needs the flexibility of locum working. She does things like pill checks, smear tests, diabetic reviews, health assessments and home visits.
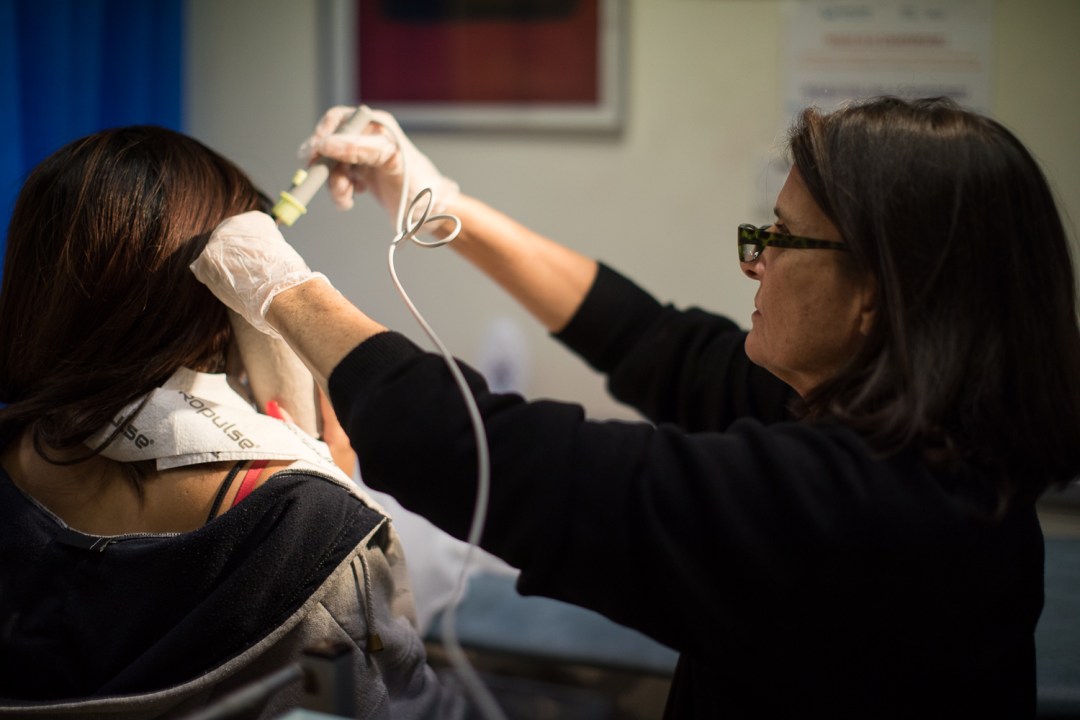
“I see a lot of stress and unhappiness,” she says. “People are working so hard just to survive. Lots of the people I meet are working multiple jobs. But then so am I. I’ve been working since I was 17 and I’ve got nothing behind me. My mum’s going to lose her house because of dementia – I’d be homeless if something went wrong.”
She says that almost all the home visits she does are to social housing tenants. “So many patients are isolated simply because they’re in buildings with no lifts – they get old and can’t get down the stairs any more.”
I join her for two visits – the first is to an 88-year-old man on the top floor of a block barely a hundred metres from the surgery. He had a stroke in July and suffers from lung disease. His wife died a few years ago and he’s now being cared for by his niece and one of his neighbours. He’s lived here since the estate was built nearly 50 years ago.

Kate’s come to take some blood for testing, but he’s lost so much weight that she can’t get a vein. A specialist team will have to come in.
In another block a little further down Lambeth Walk we meet an elderly couple, originally from Ireland, who have lived in the area since the 1950s. She’s almost bent double from crippling arthritis, walks with a frame and yet is still caring for her husband, who has dementia. We’re here because he’s due a flu jab. She’s remarkably upbeat. “You can’t complain,” she says with a smile, before offering us a cup of tea.
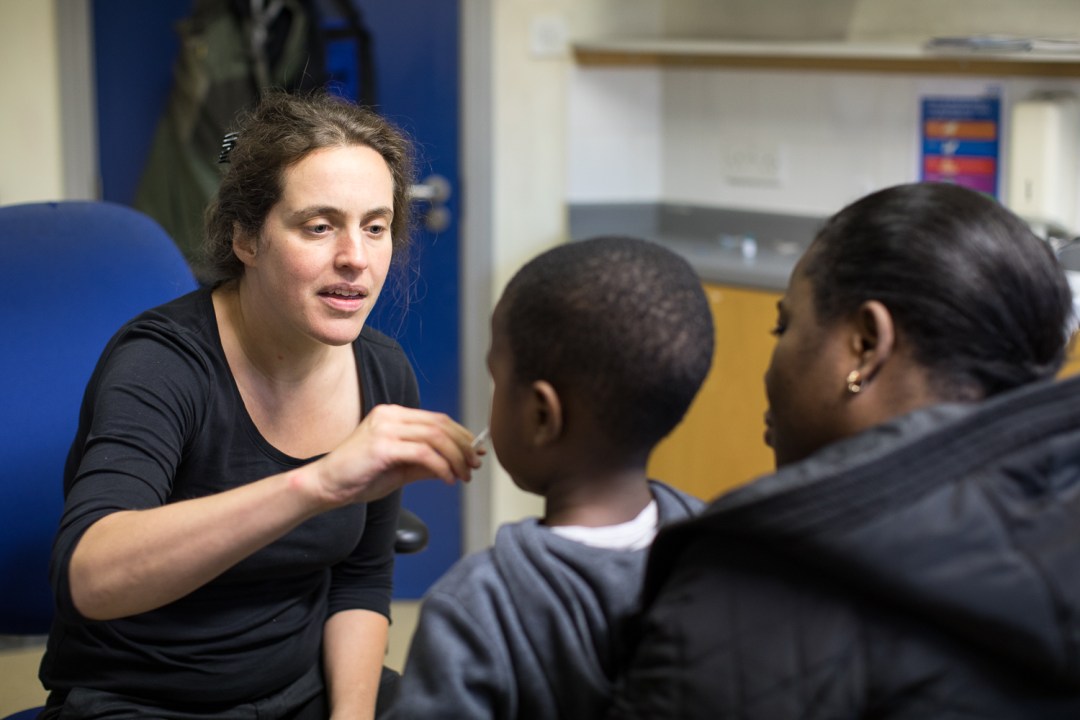
Back at the surgery, I talk to Victoria Steinhoff, another nurse practitioner. She’s giving out dozens of flu jabs today. She tells me that a lot of the people she sees are struggling to make ends meet. “I have patients that come for blood tests because they’re constantly tired,” she says. “I ask what time they go to bed and they say midnight. I ask what time they get up and they say 4am. Their cleaning job starts at 5am, they work all the way through and then the evening cleaning starts at 7pm and they work until 10. Of course they’re tired! Anyone would be. I can’t cure that.”
***
On my last day I sit down with Sarah Cross, the practice manager. She oversees the surgery’s finances and is responsible for things like patient safety, HR and the upkeep of the building. She’s been here for four years but has worked in nursing since 1992.

I’m keen to understand from her what effect cutbacks are having on the surgery itself. She tells me that things are getting harder and harder.
“Financially it’s much more of a squeeze now,” she says. “We need to repaint, we need some new chairs, but we don’t get money for anything like this, we have to pay for it ourselves – and at the moment we just can’t afford to.”
“We have less money, increasing overheads, and people have greater expectations of what we’re supposed to provide,” she continues. “But we’re not resourced for it. There are too many patients waiting to be seen. We’re being told we have to cut back and be leaner while public expectation is being increased to unrealistic levels.”
I ask why she thinks this is. “I think the agenda is to get rid of GP practices,” she replies. “I worry we’ll go the way of dentists. There are private operators snapping at our heels.”
***

A few weeks after saying my goodbyes, new data released by NHS Digital reveals a significant drop in the number of full-time GPs – down by 1,193 from the previous year. In 2015 the Government pledged to increase the number of GPs by 5,000 by 2020 to meet demand, so this doesn’t sound like a good omen.
I phone Raj to get his take on it. As well as running his surgery, he sits on Lambeth’s Clinical Commissioning Group, so he has a view of what’s happening more broadly in the borough, and beyond. He’s not surprised.
“It’s well known that there’s a national shortage of GPs,” he says, “but also radiologists, psychiatrists, paediatricians – you name it. It’s not just general practice.”
So what’s the problem? “I think the Government is very bad at workforce planning,” he says. “And I think also, because of the recent junior doctor negotiations, a lot of people are not going into training, or once they qualify they’re going abroad.”
He explains that General Practice has long been one of the less popular choices for medical students. It’s complex, intense work and sitting in a room all day by yourself can’t compete with the buzzy, social environment of a hospital, particularly for young doctors. But this has historically been less of a problem in London, where young people are keen to live and work. More recently, that has changed, he says. “Ten years ago we advertised for a GP and we got 70 applications,” he tells me. “Last time we advertised, we got two. There has definitely been a reduction in the numbers of people going into general practice.”

The other issue they face at the surgery is staff retention. Housing costs in the capital mean that doctors tend to move on once they have families. “I couldn’t afford to buy a house in Lambeth now with my salary as GP,” he says. “I’d be commuting, or I’d get a job outside London.”
The effects of the shortage are already being felt, he says, and his prognosis is not good. “I think the impact is going to be more of what we’re starting to see already,” he says. “Longer and longer waiting times to access treatment, in both primary and secondary care. And it’s going to mean more intense pressure for those of us still doing the job.”
